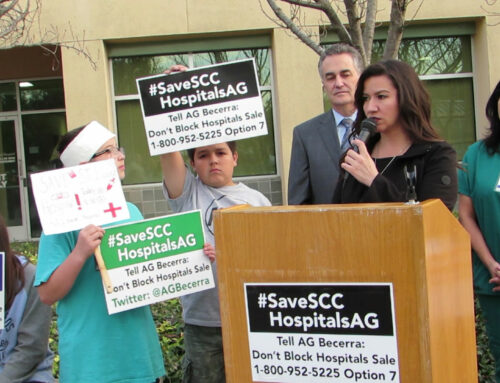Health and city officials urge residents to remain vigilant as cases surge

By Marty Cheek
The threat to the health of hundreds of thousands of people from COVID-19 is a real and growing one the public can — and must — defend itself against, Santa Clara County health officials and leaders warned at a Dec. 28 press conference.
At least 670 fatalities in the county were attributed to COVID-19 at the end of 2020, making the virus the third leading cause of death last year, over heart disease and cancer, according to public health officials.
 Over seven days around New Year’s Day, eight workers in St. Louise Regional Hospital’s emergency department tested positive for COVID-19. This is 10 percent of the ER staff.
Over seven days around New Year’s Day, eight workers in St. Louise Regional Hospital’s emergency department tested positive for COVID-19. This is 10 percent of the ER staff.
Even amid the hopeful news of expanding vaccine rollouts, the county’s hospital system remains in a precarious state with both ICU and non-ICU capacity at extremely low levels. New COVID-19 patients continue to arrive at a high rate and only 9 percent of ICU beds were available in the county as of Jan. 5. Hospital staff are stretched thin, working overtime, and weary as they provide complex care to critically ill patients.
This surge of COVID-19 patients hampers the medical system’s ability to best accommodate other incoming patients, whether for stroke, heart attack, traffic accident, or other emergency needs.
“We are still extremely worried about a surge of cases from the December holidays on top of our existing surge,” said Dr. Ahmad Kamal, Director of Healthcare System Preparedness for the County of Santa Clara.
 With a total of 93 staffed beds, St. Louise has seen an increase in the number of patients admitted to the hospital with COVID-19. Staff saw a surge of patients in December following the Thanksgiving gatherings, more than half of admitted patients have the virus. All eight beds in the intensive care unit are filled, forcing the hospital to start using surge beds.
With a total of 93 staffed beds, St. Louise has seen an increase in the number of patients admitted to the hospital with COVID-19. Staff saw a surge of patients in December following the Thanksgiving gatherings, more than half of admitted patients have the virus. All eight beds in the intensive care unit are filled, forcing the hospital to start using surge beds.
In all of Santa Clara County on Jan. 6, there were only seven ICU beds left available and zero non-ICU beds. The crisis is stressing the healthcare system to a breaking point, said Gloria Dela Merced, chief operating officer at St. Louise, at the press conference held outside at San Ysidro Park in Gilroy.
“Every day the hospitals and the county work together to support one another and manage the care of our patients,” she said. “But if the number of people with COVID-19 continues to rise, very soon all our hospitals will be out of beds and we’ll no longer be able to support each other.”
 St. Louise has mitigated some of its bed capacity issues by transferring at least 14 patients to an alternative care site recently opened at the formerly shuttered De Paul Health Center in Morgan Hill. That unit was opened in late December after a remodel by the county and is caring for patients healthy enough to leave the hospital but not yet go home. One St. Louise patient was transferred to a Monterey County hospital for care.
St. Louise has mitigated some of its bed capacity issues by transferring at least 14 patients to an alternative care site recently opened at the formerly shuttered De Paul Health Center in Morgan Hill. That unit was opened in late December after a remodel by the county and is caring for patients healthy enough to leave the hospital but not yet go home. One St. Louise patient was transferred to a Monterey County hospital for care.
Healthcare professionals every day see the seriousness of the coronavirus crisis and continue to do all they can to care for and treat patients. But it gets harder all the time, Dela Merced said. That’s why it’s vital residents of the county wear a mask in public, shelter in place, stay home if they do not have any essential needs, and wash their hands to take care of each other.
“If we go beyond the surge capacity, everyone will be affected,” she said. “More people will know someone who died or who is seriously ill. We do not want this to happen, but I worry every day that it may happen.”
 Gilroy Mayor Marie Blankley also emphasized at the press conference the need for members of the public to heed the warnings of health experts that the best way to face the threat of COVID-19 is to take actions that lessen the opportunities for the virus to spread.
Gilroy Mayor Marie Blankley also emphasized at the press conference the need for members of the public to heed the warnings of health experts that the best way to face the threat of COVID-19 is to take actions that lessen the opportunities for the virus to spread.
“I’m here to ask that everybody get out of our own heads and out of our own little bubble and instead think more frequently about all the people around us who are being affected in many different ways — some have lost family members, some have lost their livelihoods, some are losing their spirit,” she said.
Depending on jobs and livelihoods, individuals may be more susceptible in their environment if they do not have the luxury to work from home, she said. That’s making it difficult for some people to not contract the virus.
In Santa Clara County, the Latino community is by far the most affected population hit by COVID-19. The data shows that 52 percent of all confirmed cases are made up of people in this group, which represents only about a quarter of the county’s population.
One of the reasons why Latinos are so severely at risk is that many in this demographic group work in jobs that force them to face a greater exposure to the virus. They also live in households where other adults make their livelihoods where they are more susceptible to catching the coronavirus.
 Gilroy’s population is about 55 percent Latino, the highest in the county. The city has had about 10 percent of its residents listed on the toll of confirmed COVID-19 cases, with as many as 25 people dead from the disease last year, according to the county. Compare that to Morgan Hill with 5 percent of its population as confirmed cases and zero coronavirus deaths in 2020, according to the county.
Gilroy’s population is about 55 percent Latino, the highest in the county. The city has had about 10 percent of its residents listed on the toll of confirmed COVID-19 cases, with as many as 25 people dead from the disease last year, according to the county. Compare that to Morgan Hill with 5 percent of its population as confirmed cases and zero coronavirus deaths in 2020, according to the county.
An insidious quality of the virus is in many cases people do not know they have it. Just because an individual does not show signs of the coronavirus — such as high temperatures, trouble breathing, nausea or vomiting — does not mean that they are not carrying the microbe and might still spread it. At least 40 percent of people with COVID-19 do not experience symptoms while still being contagious, according to the county’s public health department.
Many Latino men and women work in jobs where they can be exposed to the virus because of operating conditions. In late May, nearly 40 cases of coronavirus were traced to workers at Lusaamerica Foods, a Morgan Hill-based fish-packing company.
 Latinos work in jobs where they may not have the luxury to work from home, said Yvonne Beltran Martinez, a Morgan Hill city councilmember. There are many reasons why this group is more susceptible to the virus.
Latinos work in jobs where they may not have the luxury to work from home, said Yvonne Beltran Martinez, a Morgan Hill city councilmember. There are many reasons why this group is more susceptible to the virus.
Their job may be essential and multiple people in their homes may be essential, which requires them to work with others or work in other people’s space, increasing your chances of getting COVID-19, she said.
“You may not have a car or second car and must use public transportation or depend on others for rides,” she said. “Perhaps you don’t have the Internet at home or access to printed materials for school. You might not be able to afford for a parent to stay home or childcare and must leave kids with a relative or a friend, increasing your exposure.”
Many firefighters in the county have received vaccination shots because they are considered essential healthcare workers, said Christina Turner, city manager for Morgan Hill.
The year 2020 has been one that people will not soon forget, with many challenges that no one could have imagined, she said. Despite these challenges, people helped each other in a spirit to make the future brighter.
 “Throughout the year, you have rallied to support our businesses, our restaurants, and our nonprofits have organized to take care of those in need,” she said at the press conference. “Individually, you have reached out to take care of neighbors and friends. Despite the losses and challenges, we have not lost our spirit. Morgan Hill and Gilroy as well as the county have worked to keep our community safe. We encourage you to hold on to hope.”
“Throughout the year, you have rallied to support our businesses, our restaurants, and our nonprofits have organized to take care of those in need,” she said at the press conference. “Individually, you have reached out to take care of neighbors and friends. Despite the losses and challenges, we have not lost our spirit. Morgan Hill and Gilroy as well as the county have worked to keep our community safe. We encourage you to hold on to hope.”